Arms race
It’s not only committed anti-vaxxers who are unwilling to have the Covid-19 jab – it’s others with more legitimate concerns. The key to the vaccine’s success is to listen to them say health experts
Work is needed to persuade the “vaccine cautious” to take the Covid-19 jab and help the UK return to greater normality, it has been warned.
Doctors and scientists say some sections of the population need convincing the vaccines are safe and that corners have not been cut in their development or approval.
The World Health Organisation says society is fighting an “infodemic” alongside the pandemic – with a deluge of information making it difficult to discern fact from fiction.
“While people’s reasons can be quite varied, they normally centre on the issue of trust.”
Those who believe wild online conspiracies – such as the vaccine being a ploy to implant microchips – may be relatively few in number, but fake news is everywhere and scepticism is widespread. Social media is full of people expressing doubts about the speed of its development and possible side-effects. Many are not anti-vaxxers but some may have been influenced by false or misleading information.
England’s chief medical officer, Professor Chris Whitty, believes a small cohort will never be convinced and are not worth worrying about in public communication terms.
“There are a lot of [other] people, though, who actually have quite legitimate questions of any vaccine and any medical treatment,” he told a joint session of the Commons Science and Technology and Health and Social Care committees. “A lot of the people are waiting to see and I think with the right information they will think, yes actually, this feels right to me.”
Vaccines protect the individual and also, if take-up is great enough, contribute to herd immunity. Last week the National Audit Office said the government would spend nearly £12 billion on buying vaccines. The level of coverage required depends on the effectiveness of any given product but NHS England would like the Covid-19 programme to reach 75 per cent of adults. In the short term, however, the programme will use early vaccine supplies to protect those most vulnerable to the disease.
Junior doctor Parth Patel worked on the frontline during the early months of the pandemic, before joining the Institute of Public Policy Research as a research fellow. He is also a clinical research fellow at University College London, where he is looking at ethnic disparities in Covid-19, including vaccine hesitancy.
He says: “The first rule with all vaccine hesitancy is to shut up and listen to the other person. Most concerns are legitimate, whether someone is being branded as an anti-vaxxer or as vaccine hesitant. Each community has its own nuances and concerns. While people’s reasons can be quite varied, they normally centre on the issue of trust – not a mistrust of science necessarily but
trust in authority, in institutions and in the state.”
Vaccines started being rolled out in hospitals and GP surgeries in December, but some have opted out. Two groups of GP practices in Manchester – which together have 100,000 patients – are among those that will not take part due to concerns they would not also be able to maintain other services for patients. Last week the Commons Public Accounts Committee said that Public Health England felt it had been shut out of important decisions despite being a health body with substantial experience of vaccination programmes.
Last month, a poll by JL Partners found women were most cautious about the vaccine – with 20 per cent unwilling to take it, compared with 16 per cent of men. Seventy per cent of women said they would definitely get vaccinated, compared with 78 per cent of men. In the North West, 49 per cent of respondents believed the Pfizer BioNTech vaccine – so far the only candidate to be approved in the UK – had been rushed, while in Yorkshire and Humberside, the figure
was 59 per cent.
Dr Heidi Larson, director of the Vaccine Confidence Project and an anthropologist from the London School of Hygiene and Tropical Medicine, told a recent online lecture: “Rumours, conspiracies and uncertainty thrive in uncertain situations like a new virus. I think unfortunately these groups that are anti-mask and anti-lockdown are converging with people who are anti-vaccine and it’s not even about the specifics about the vaccine – it’s about an underlying distrust.
“The scientific community and medical community generally have taken public trust for granted. There’s been disproportionate investment into new vaccines and pennies into public engagement. We need more listening and to be willing to have a conversation even when we don’t necessarily agree.”
Dr Tom Fletcher, from Liverpool School of Tropical Medicine (LSTM), has worked on disease outbreaks in regions such as West Africa and believes communication is key. During the Ebola crisis, health workers engaged with community leaders, who then helped deliver messages into communities.
“The community needs to understand why you’re there and what you’re putting in place in order to stop chains of transmission,” he says. “If they don’t or if they remain in denial or have distrust of authority or health services, you’ll never win. This communication must be done in the right way. I’m not sure if we’ve done that as well as we need to so far.”
One frequent concern relates to the pace of vaccine development – with online commentators constantly repeating the claim that vaccines normally take seven-plus years to produce. Another is that drug companies have been exempted from civic liability if vaccines are later found to cause harm. Both have simple explanations but in the climate of suspicion and half-truth it is difficult to persuade sceptics otherwise.
Although she believes the number of ideological anti-vaxxers is probably quite small, Dr Cheryl Walter, a virologist from the University of Hull, has concerns that low take-up of this vaccine could make our return to normality very slow indeed.
She thinks scientists and public health officials should be open about the data and keep pointing out that any risk of harm from a vaccine is dwarfed by the potential impact of catching Covid-19.
“In a way I think it’s good that people question processes and data and I would never discourage that, but I think often we’re not really thinking about how the relatively mild side effects from a vaccine – things like fever for a short time – compare to Covid-19 itself,” she says.
“I think the communications response needs to be coordinated – perhaps something like a letter signed by virologists, vaccinologists, doctors and public health officials, summing up what the advantages of the vaccine are, why we think it’s a good idea and the fact we’d be at the front of the line to get a jab.”
Support for vaccines ebbs and flows, even when they’ve been around for years and been proven safe and effective. The 1998 Andrew Wakefield scandal – which falsely linked the measles, mumps and rubella jab with autism – did huge damage to childhood vaccination rates. There are still periodic surges of measles and other illnesses when inoculation rates dip.
Fletcher says: “With the Covid-19 vaccine there’s a societal benefit to getting it. Although you may decide not to have it and feel you are making an informed decision, unfortunately you are posing a risk to people who are more vulnerable and don’t have that choice. That’s the problem I have with this group of patients who don’t want intervention and won’t make the behavioural changes they are being asked to.
“On a personal level that’s fine but on a community level it’s not. They pose a risk of transmission to people who may well die. How we frame that argument and get it across to all sections of the population is now key.
“In places like Liverpool where some communities are very hard hit by Covid-19, people shouldn’t need too much convincing to take the vaccine. You would hope so, anyway.”
Research shows there are particular sections of society that may be more cautious about the vaccine – including some who are especially vulnerable to Covid-19 due to structural inequalities.
A survey by the Vaccine Confidence Project and Public Health England found people from ethnic minority backgrounds were almost three times more likely to reject a Covid-19 vaccine than those from white backgrounds. Participants from lower-income households were also more likely to reject the idea than those from more affluent households – with some saying they wanted to wait and see if the vaccine was safe before taking part.
The report warns: “The success of Covid-19 vaccination programmes will rely heavily on public willingness to accept the vaccine.
“Importantly, efforts must be made to understand and address factors that may affect Covid-19 vaccine uptake in black, Asian and ethnic minority groups and lower-income households who are disproportionately affected by Covid-19.”
Efforts are being made to bring communities on board with targeted approaches. Bradford Royal Infirmary is working with community leaders to devise ways to encourage the city’s large Asian population to have the jab. Religious figures across the country are being asked for help persuading congregations that the vaccine is good for society as a whole.
The Muslim Council of Britain is partnering with the British Islamic Medical Association to encourage adherents to take up the offer of a flu vaccine this winter, following a dip in rates. Since flu weakens the immune system, it can leave people open to contracting other infections such as Covid-19 or pneumonia.
“With Muslim communities having higher mortality rates of Covid-19 than any other faith group, flu threatens to further impact the health of our communities,” reads the accompanying text.
Bradford West MP Naz Shah has taken part in Covid vaccine trials in the hope of increasing trust in the system among minority communities, along with equalities minister Kemi Badenoch. Medical trials traditionally struggle to recruit participants from minority ethnic backgrounds – a fact that does little to engender trust in the resulting vaccines.
Patel says the choice of messenger is as important as what is being said when it comes to bringing communities on board.
“The usual reflexive way to react is to assume that people don’t have the right information, that they operate in information vacuums,” he says.
“What people forget is that the important part is to listen. It’s not just the information that matters – it’s also how you deliver it and who delivers it. Messenger, arguably, is as important as message. Communication coming from the local GP will have a different impact than information coming through central diktat.
“I believe GPs are best placed to do this. They are local, they are community leaders, and in rural areas in particular they are well known. They are experienced with delivering vaccines and they are trained listeners.”
NHS England, which is running the vaccination programme, is trying to use primary care as much as possible, despite the logistical challenges posed by the Pfizer BioNTech vaccine, which must be stored at minus 70 degrees and spoils within days once defrosted.
The other important thing to remember is that there may be stated hesitancy around the vaccine, but that may not translate into behaviour, Patel adds.
“It’s not a direct jump from one to another,” he says. “People may tell a researcher that they won’t take a vaccine or write it on social media, but when their GP calls them in to have it they may act differently. If the information is coming from someone they trust, they are more likely to believe it.”
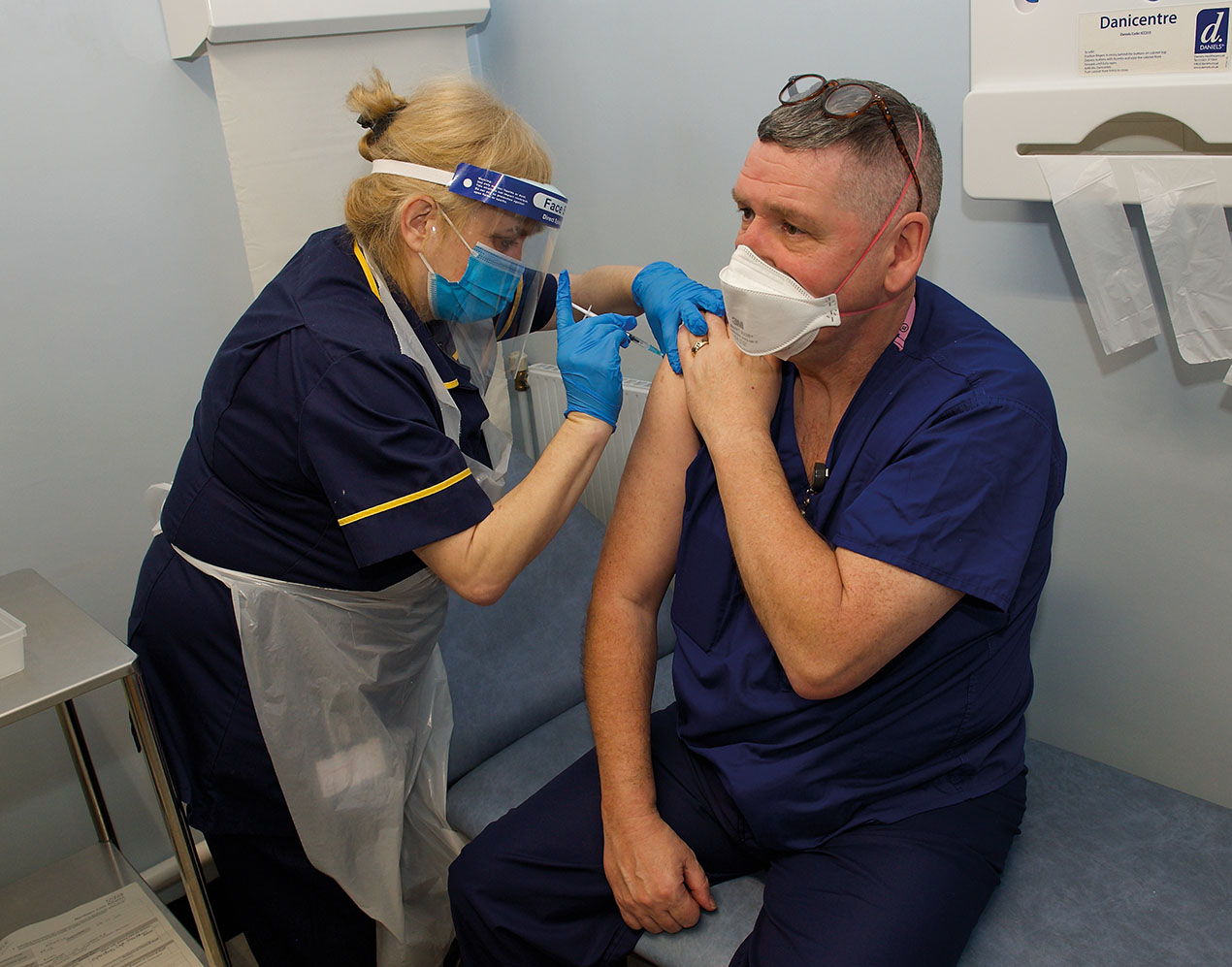
Main image: NHS worker Mick Newell receives a Covid-19 vaccination at Salford Royal Hospital on the first day of the largest immunisation programme in UK history (PA)
Many Covid vaccine sceptics regard the fact that pharmaceutical firms have been exempted from civil liability as proof they are unsafe. The exemption protects firms from liability if the government rolls out their products without licensing, as it has with the Pfizer BioNTech jab. They are not exempt from all liabilities, but without this change the vaccine may not have been forthcoming.
Experts say all safety steps have been followed, and scientists from the Medicines and Healthcare Products Regulatory Agency (MHRA) – which is independent of government – have scrupulously combed through the data.
The pandemic is an unprecedented situation. With hundreds of millions of people due to be immunised globally, the question of who pays for damages in case of side-effects has been a huge issue in supply negotiations.
In the UK and the EU, exemptions can be granted to companies when medicines are fast-tracked because of emergencies.
“This is a unique situation where we as a company simply cannot take [on] the risk,” Ruud Dobber, a member of Astra Zeneca’s senior executive team, told Reuters.
His firm is awaiting approval for its vaccine developed with Oxford University. “In the contracts we have in place, we are asking for indemnification. For most countries it is acceptable to take that risk on their shoulders because it is in their national interest.”
Far from being something to worry about, experts believe the pace of Covid-19 vaccine development should be something to celebrate.
Normally the process is held up for years by funding bids, funding refusals, more funding bids, submissions to ethics boards, regulatory delays, trial volunteer recruitment and dealing with drug companies. This time, the technology already existed, ample funding was available and there was unprecedented international scientific collaboration, with steps that normally happen in sequence taking place in parallel.
Dr Cheryl Walter, Hull University virologist, says: “The foundation of the Pfizer BioNTech vaccine came from Sars Coronavirus 1, which came and went and so did the money. Now we’ve had a huge financial investment and managed to make multiple breakthroughs with clear scientific evidence. I thought it would take 18 months to two years but it’s happened way faster. It’s an amazing achievement.”